September 15, 1993
Dear Colleague,
During the June shipping cycle for the DNA typing project, we received approximately 3000 frozen cell samples. The continued support of all participating laboratories is greatly appreciated. To clarify misunderstandings, the main purpose of the DNA project is not the determination of error rates in serological HLA-DR typing anymore. Conclusive information on this topic was obtained and published both in this newsletter and in the literature. The DNA typing technology is spreading rapidly and an increasing number of laboratories are reporting HLA-DR results based on this technique. We are pleased that the availability of CTS "String Kits" for rapid DNA-SSP typing is contributing to this development.
As for the collaborative DNA project for which frozen samples are solicited, the emphasis has shifted towards the characterization of additional HLA loci. Currently, large scale typing is being done to determine the influence of HLA-DQA, HLA-DQB and HLA-DP on graft outcome. Moreover, as methods are becoming available for the DNA determination of HLA Class I (HLA-A, HLA-B, HLA-C), we will include testing for these loci in the study. Please support this collaborative project which is certain to result in very valuable information. We would appreciate it very much if you would continue to freeze recipient blood samples and donor spleen tissue. The next shipping date will be February 7 or 8, 1994.
_______________
During the last year we have struggled with the problem of equitable kidney allocation. A strong effect of HLA matching on cadaver kidney survival has repeatedly been shown in this newsletter. However, if kidneys were allocated strictly according to the best possible HLA match, patients with rare HLA phenotypes would be at a disadvantage. This would especially affect racial minorities. Thomas Wujciak performed extensive computer simulations and developed a weighted point system which is self-adjusting to the dynamics of a waiting list. His initial results were published a few months ago and he has since been able to improve the allocation model. It now takes the following parameters into account: HLA-A,-B,-DR match, waiting time, race, priority of local transplant, kidney exchange balance for each center, and probability for a 0-1 HLA-A,-B,-DR mismatch in 1000 kidney offers ("matchability"). The exact details of the allocation algorithm are available to anyone who is interested. The following graphics show the power of the newest version, termed "XCOMB". Waiting list conditions and donor availability were chosen as realistic , as possible based on information published by Eurotransplant and UNOS, and on HLA frequencies derived from the CTS file. The results were simulated over a 6-year period, assuming that the best suitable patient would be transplanted in only 50% of the selections.
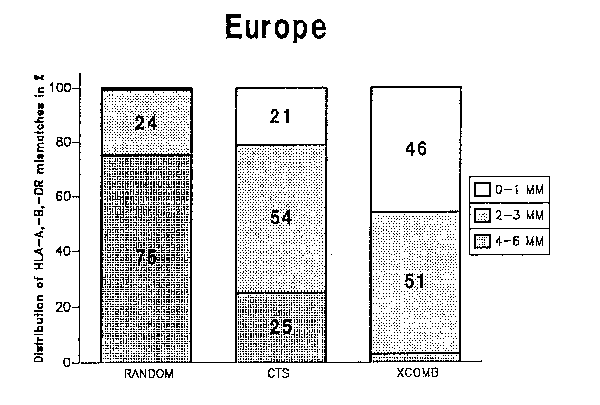
Figure 1 shows the fractions of different HLA-A,-B,-DR match grades that can be obtained in Europe with random allocation and the XCOMB allocation method. The actual results reported by European centers to the CTS study are shown for comparison. It is evident that the fraction of good matches can be improved by means of organ allocation by the XCOMB method. The corresponding results for North American Caucasians are shown in Figure 2, and those for African Americans in Figure 3.

Figure 1
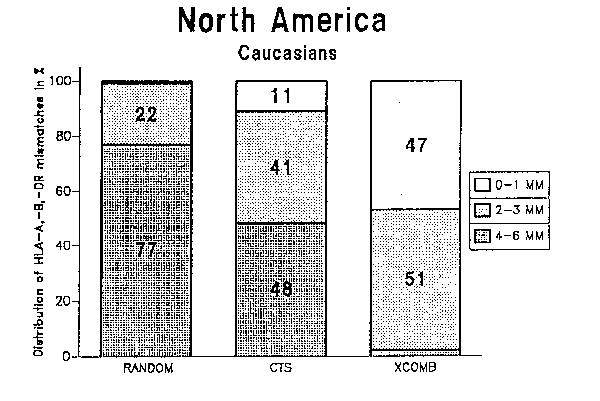
Figure 2
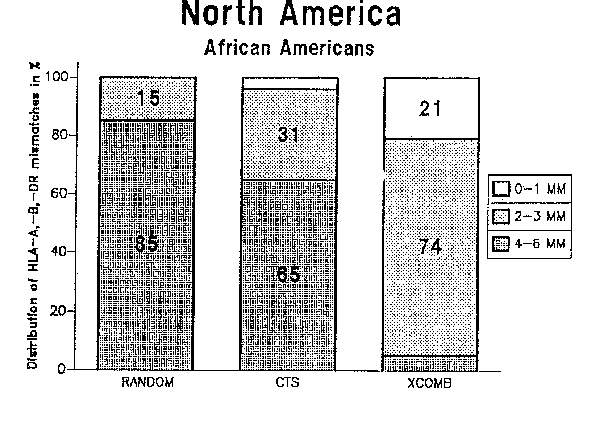
Figure 3
Because the XCOMB method considers the likelihood for a patient to receive a better match in the future, the overall likelihood for all patients in the waiting pool to receive good matches does not decrease with time. This is an important difference to strict HLA oriented allocation, which selects for patients with "easily matchable" HLA antigens and leads to an accumulation of patients with rare antigens (Figure 4). Moreover, the mean waiting time of all patients in the pool also evolves more favorably with the XCOMB method as compared to strict allocation by the HLA match (Figure 5). Perhaps most importantly, the maximum waiting time can be reduced dramatically (Figure 6). Since patients with extremely rare phenotypes are given special consideration, they are not left waiting for "perfect matches" but receive "reasonable" matches fairly quickly.
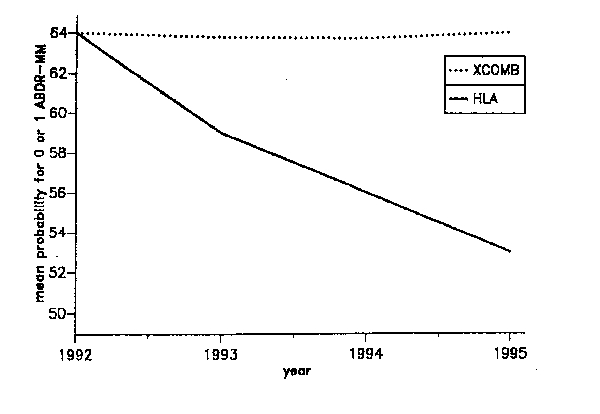
Figure 4
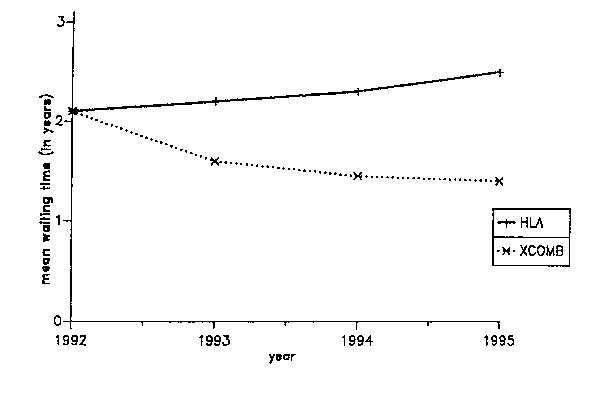
Figure 5
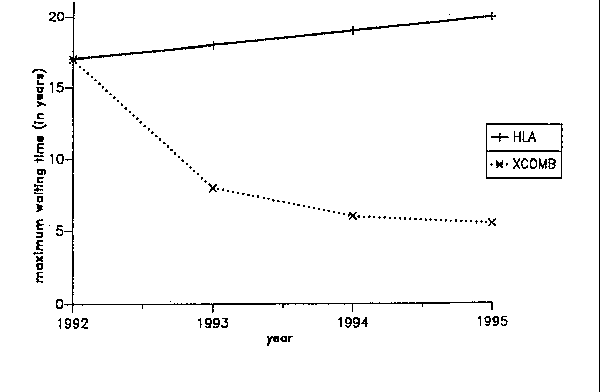
Figure 6
We believe this model is superior to the allocation methods currently used. It can be expanded to include additional variables, such as priority for pediatric recipients, the patient's presensitization status, or even the geographical distance between centers. Naturally, the model is not very effective with small waiting lists. The model's advantage is clearly demonstrable with a waiting list of 1000 patients, and it gains power as the waiting list increases to 10,000 patients. Although the model has been tested in computer simulations only, it has performed very impressively. Hopefully, the method will be put to practical use and contribute to an improved allocation of cadaver organs.
Thank you for your continued support.
Sincerely yours,