Figure 1
November 1, 2010
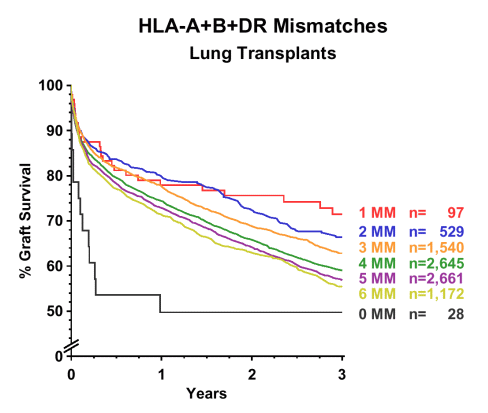
We recently made the curious observation that HLA matching in lung transplantation shows a strong correlation with outcome but, paradoxically, the small group of patients with perfectly matched transplants (zero A+B+DR mismatches) experienced a particularly high early graft failure rate. This finding is reminiscent of reports in the literature demonstrating a high rate of graft failure in well matched liver transplants (Markus et al. Transplantation 1988, 46:372, and Donaldson et al. Hepatology 1993, 17:1008). The phenomenon was attributed to "HLA restriction", meaning that certain autoimmune processes or infections are favored by identical HLA characteristics in the recipient and the donor. The CTS lung transplant data are shown in Figure 1. Although only twenty eight 0- mismatch lung transplants were available for analysis, their outcome was significantly worse than that of the HLA mismatched groups (P < 0.001).

Figure 1
It is disappointing that our analysis of the CTS liver transplant data did not show a clear HLA restriction effect. There was no correlation between HLA matching and liver graft outcome (Figure 2). It is possible that a subgroup analysis of patients according to underlying disease (e.g. autoimmune or not) may be necessary to uncover the HLA restriction phenomenon but our attempts to do this, while admittedly crude, did not yield convincing results (not shown).
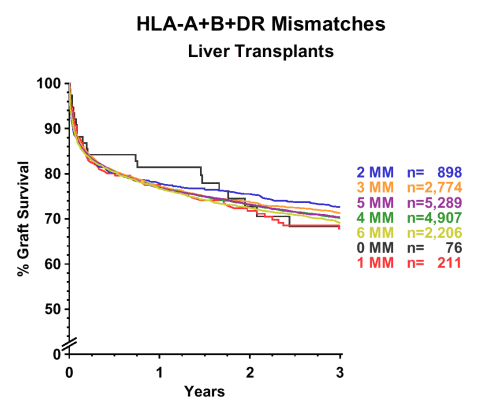
Figure 2
Interestingly, we found evidence suggesting that an HLA restriction phenomenon may be present in heart transplantation. In our previous analyses, we combined the 0- and 1-mismatch groups because patient numbers were relatively small compared to the groups with more HLA mismatches. When the recent lung transplant results prompted a more detailed analysis of outcomes in heart transplants, it became apparent that grafts with 0 or 1 HLA A+B+DR mismatch behaved quite differently from one another. Whereas the 1 mismatch group showed a superior survival rate as expected, the survival curve for grafts with 0 mismatches demonstrated an unusual evolution, declining during follow up to meet the curve for 6-mismatch transplants (Figure 3). It therefore seems conceivable that some form of HLA restriction may be operative in heart transplantation, although perhaps only in a subgroup of recipients.
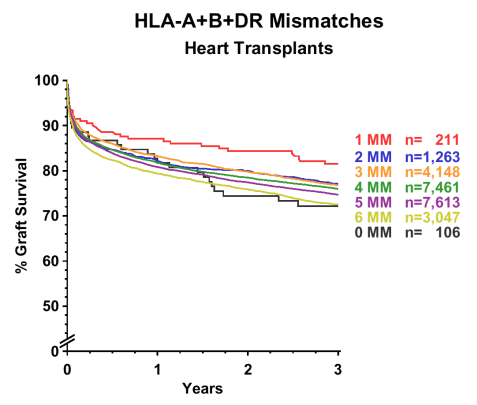
Figure 3
These data suggest that the analysis of HLA matching in organ transplantation may be complicated by a "counteractive" HLA restriction phenomenon. The effect appears more readily identifiable in situations of "perfect" HLA compatibility, although we are not aware of a group of kidney transplants in whom the HLA restriction phenomenon is apparent. Subgroup analysis may be a promising method of elucidating the clinical significance of this fascinating biological phenomenon in clinical transplantation.
I should like to point out that these interesting observations were possible only because we have compiled a unique data base, the result of a remarkable collaborative research project of nearly 30 years duration, founded entirely on the voluntary support of all of you. Thanks are due to everyone who has contributed!
Thank you for your continued support of the CTS study.
Sincerely yours,